 Incredible Marketing
Incredible MarketingSUPERFICIAL RADIOTHERAPY OR SRT FOR SKIN CANCER

Superficial Radiotherapy or SRT is a safe, painless and effective FDA-approved modality to treat non-melanoma skin cancer such as basal cell carcinoma or squamous cell carcinoma, virtually any place on the body. SRT is not like the radiation used to treat other cancers. The SRT Technology and the SRT-100™ Treatment System are specifically designed to treat Skin Cancer! Unlike the other more powerful radiation devices used for treating other cancers, SRT is designed to only penetrate up to 5mm below the surface of your skin. It preserves the surrounding healthy tissue while effectively treating the malignant skin cancer cells. In other words, Superficial Radiotherapy (SRT) is a proven non-surgical choice that goes no deeper than the thickness of the skin. Most recently, Sensus Healthcare LLC, manufacturer of SRT-100 received coveted 2014 North American Frost & Sullivan Award for New Product Innovation Leadership Award.
Dr. William Ting is proud to be among the first dermatologists in California and San Francisco Bay Area to introduce SRT-100 non-surgical radiotherapy treatment for nonmelanoma skin cancers such as basal cell carcinoma or squamous cell carcinoma with a state of the art radiotherapy suite. Dr. Ting is licensed by the State of California as a Physician Supervisor and Operator of Dermatology-related Superficial Radiotherapy. Along with his radiation therapist Hallie Gremlitz R.T. board-certified through the American Registry of Radiologic Technologists and a member of the American Society for Radiologic Technologists, Dr. Ting has provided thousands of fractionated superficial radiotherapy treatments and arguably has the most amount of experience treating resistant keloid and hypertrophic scars in California and the West Coast. To date the rate of recurrence of non-melanoma skin cancer treated with SRT at our facility is less than 0.5%.
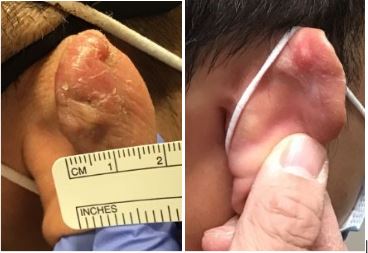
Before and After photos of a keloid treated with shave excision and SRT
Click here to view the SRT Keloid Before and Afters
WHY CHOOSE SUPERFICIAL RADIOTHERAPY?
The majority of skin cancers (more than 50%) occur in those over the age of 60. While the traditional treatment path for non-melanoma skin cancer has been Mohs surgery, this population has a high incidence of risk for surgical procedures due to underlying conditions such as diabetes or heart disease, which can slow the healing process. Mohs surgery involves a series of excisions to remove cancerous tissue and surrounding healthy tissue until the cancer can no longer be detected. This procedure can also lead to substantial cosmetic surgery requirements and a drawn-out healing process that may result in infection, making it unsuitable for many skin cancer patients.
SRT-100™ offers a different solution for non-melanoma skin cancer treatment for those who have a high surgery risk. Because 80 percent of skin cancers occur in the head and neck regions, where surgery would require great tissue loss and significant cosmetic repair, the SRT-100™ by Sensus looked to a proven technique that goes no deeper than the thickness of the skin to effectively treat non-melanoma skin cancer. Known as low energy radiotherapy, this technology has been in use for more than 50 years.
Compared to the legacy orthovoltage systems that are used in some dermatology and radiation oncology practices, Sensus offers the SRT-100™ as a modern solution, which is a safe, effective, and reliable technology for efficient treatment of non-melanoma skin cancers.
IS THE SRT-100™ A SAFE TREATMENT OPTION?
The SRT-100™ is a proven technology for treating non-melanoma skin cancers, actinic keratosis, and Kaposi’s sarcoma. It is safe and highly effective. It is utilized by dermatologists and radiation oncologists all over the world as a proven treatment with proven outcomes. During each fractionated treatment session, the patient will be fully shielded with protective lead equipment. There is no scattered radiation emitted from SRT-100™ and the state-of-the-art lead-shielded radiotherapy suite is certified by a licensed physicist.
ADVANTAGES OF SUPERFICIAL RADIOTHERAPY
Because the superficial x-rays concentrate radiation dose on the skin surface, SRT-100™ treatment has several advantages over surgical procedures for non-melanoma skin cancers. These advantages include:
- Safe & Effective
- Same results as surgery without the pain
- Very short treatment sessions
- Virtually painless / no cutting
- Minimal to no scarring / no stitching
- Virtually no risk of nerve damage
- No anesthesia required
- Virtually no post-surgical infections
- Faster healing process
- No post reconstructive surgery required
- High cure rates
- No down time – you can still shower, play golf, tennis etc.!
Click here to view the SRT Skin Cancer Before and Afters
SUPERFICIAL RADIOTHERAPY FOR KELOID SCARS
Superficial radiotherapy (SRT) utilizing SRT-100TM by Sensus Healthcare, is the most revolutionary new modality for keloid and hypertrophic scar. This FDA-approved therapy is among the most effective procedures to treat even the toughest keloid. While SRT-100TM can be used to treat keloid without incision utilizing a protocol of one SRT session per week for 4 weeks in a row, SRT modality has the highest success rate (in excess of 90%) when it is performed once daily, 3 days in a row, preferably within 24 hours of surgical excision of the original keloid skin tissue. Most treated patients will experience concurrent reduction or itching and pain associated with keloids. SRT has much greater safety margins compared to traditional orthovoltage radiation therapy as SRT involves typically one thousand times less energy, no associated radioactivity or scattered radiation. Side effects associated with SRT for keloids are usually minimal and may include pigmentary changes in the treated area. SRT for keloid is typically covered by most PPO insurance carriers (subject to typical copay, deductible and coinsurance) and Medicare though preauthorization may be required. Any residual keloid tissue after SRT can be further flattened with intralesional 5-fluorouracil/cortisone injection at later date. Dr. Ting and the clinical team at California Dermatology Care is among the first dermatologists in California and West Coast to administer this state-of-the-art technology for keloid and arguably may be among the most experienced medical clinics in the nation in administering SRT for keloids.
Compared to traditional orthovoltage radiation therapy, SRT typically involves a thousand times less energy and no associated radioactivity or scattered radiation, giving it much greater safety margins. Side effects associated with SRT for keloids are usually minimal and may include pigmentary changes in the treated area. Any residual keloid tissue after SRT can be further flattened with intralesional 5-fluorouracil/cortisone injection at a later date. Dr. Ting and the clinical team at California Dermatology Care are among the first dermatologists on the West Coast to administer this state-of-the-art technology for keloids and may arguably be among the most experienced medical clinics in the nation in administering SRT.
SRT for keloid is typically covered by most PPO insurance carriers (subject to copay, deductibles and coinsurance) and Medicare, though preauthorization may be required.
IL 5-FU FOR KELOIDS AND SKIN CANCER
Another option for the non-surgical management of certain skin cancers is the chemotherapy drug 5-fluorouracil (5-FU). While most cancer treatments involve a systematic or surgical approach to eliminate cancer cells, intralesional (IL) 5-FU is a minimally-invasive technique that delivers the medication directly into cancerous lesions. It works by inhibiting DNA synthesis and has proven to be a viable treatment option for those who are poor candidates for surgery, providing favorable outcomes with no significant side effects or scarring. Although the exact approach used varies with each patient, intralesional injections are typically given once or twice weekly and often require somewhere between four to eight treatments until clinically clear.
Chemotherapeutic drugs like 5-FU are also used to treat keloid scars. Keloids are a type of thick, fibrous scar that forms due to a faulty or disrupted wound healing process. Keloid scars develop after an injury to the skin, such as a cut, scrape or insect bite, and can appear anywhere on the body. It can take weeks or months for a keloid to grow and they often end up much larger than the original wound. Despite a variety of therapeutic options available for keloid scar treatment, they remain a challenge for many patients and providers.
IL 5-FU and cortisone injections have been shown to effectively flatten and improve the appearance of keloid scars, especially those that are stubborn or recurring. While other treatment modalities can help remove keloids, they do not suppress keloid growth and scarring may reappear at a later date. IL 5-FU inhibits the proliferation of fibroblasts, the main cells involved in keloid formation, resulting in much lower rates of recurrence after treatment. IL-FU/cortisone injections can also help eliminate residual keloid tissue after SRT or surgical removal. Much like with IL 5-FU for cancerous lesions, this treatment can effectively treat keloids with few significant side effects, but patients are monitored for any adverse reactions. Drug dosages are adjusted for each patient for a safe and sustainable treatment option.
FREQUENTLY ASKED QUESTIONS
What kind of conditions can be treated by the SRT-100™?
The SRT-100TM is an excellent treatment option for patients with the following conditions:
- Basal Cell Carcinoma
- Squamous Cell Carcinom
- Metatypical Carcinoma
- Cutaneous Appendage Carcinoma
- Kaposi’s Sarcoma
- Advanced Hypertrophic Actinic Keratosis
- Keloid
Why is the SRT-100™ a viable alternative to surgery?
The SRT-100™ doesn’t harm surrounding or underlying healthy tissue while targeting only the cancer.
What should I expect from SRT-100 treatment?
You should expect the same results as surgery without the following:
- No pain
- No anesthesia
- No cutting
- No bleeding
- No stitching
- No scarring
Is SRT-100™ a safe treatment option?
The SRT-100™ is proven technology to treat non-melanoma skin cancers, actinic keratosis, and Kaposi’s sarcoma. It is safe and proven effective. It is utilized by dermatologists and radiation oncologists all over the world as a proven treatment with proven outcomes. During each fractionated treatment session, the patient will be fully shielded with protective lead equipments. There is no scattered radiation emitted from SRT-100™ and the state-of-the-art lead-shielded radiotherapy suite is certified by a licensed physicist.
How long is a typical treatment?
Depending on the treatment protocol Dr. Ting chooses for your particular case, you may be required to have 2-3 treatments per week for up to 4-5 weeks. Each treatment can last as long as 50 seconds.
What is the cure rate of Basal & Squamous Cell skin cancer when treated with the SRT-100™?
The SRT-100™ has a cure rate of 95% to 98%.
Will I need reconstructive surgery post treatment?
No. The SRT-100™ is a non-invasive procedure.
Is Superficial Radiotherapy utilizing SRT-100 technology covered by my health insurance carrier?
Radiotherapy for non-melanoma skin cancer is medically necessary and is covered by Medicare and most PPO private health insurance carriers. No preauthorization may be necessary for Medicare patients. For private health insurance carriers, our office will work with you to get pre-certification/pre-authorization for SRT. Your out-of-pocket expense would depend on your deductible and co-insurance.
Why Low Energy Radiotherapy?
Over 50% of skin cancers occur in those over 60. This population also has a high incidence of risk for surgical procedures due to various disorders like diabetes and cardiac diseases that can slow the healing process. The traditional treatment path for non-melanoma skin cancer has been Mohs surgery. This surgery involves a series of excisions of cancerous tissue and surrounding healthy tissue until the cancer can no longer be detected. This procedure can lead to substantial cosmetic surgery requirements and a drawn-out healing process which can result in infection. SRT-100™ offers a different solution for non-melanoma skin cancer treatment for those who have a high surgery risk. Because 80 percent of skin cancers occur in the head and neck regions, where surgery would require great tissue loss and significant cosmetic repair after surgery, SRT-100 by Sensus looked to a 50-year proven technique, known as low energy radiotherapy which goes no deeper than the thickness of the skin to effectively treat non-melanoma skin cancer.
Compared to the legacy orthovoltage systems that were used in the dermatology and radiation oncology practices, Sensus offers the SRT-100™ as a modern solution, which is a safe, effective, and reliable technology for efficient treatment of non-melanoma skin cancers.
How doesXoft™ Electron Brachytherapy differ from SRT-100™ Superficial Radiotherapy for radiation treatment of non-melanoma skin cancer?
Electron Brachytherapy using Xoft™ is a fine technology but utilizes more potent electron beam that was initially designed to penetrate body cavities as well as for radiation treatment of prostate cancer and breast cancer. Given the potency of Electron Brachytherapy (EBX), it must be administered under direct supervision of Radiation Oncologist during each fractionated treatment to minimize accidental or inadvertent injury. The major advantages of SRT-100™ Superficial Radiotherapy over Xoft™ Brachytherapy are much lower cost to the health care system as well as continuity of care with your Dermatologist who is licensed via State of California to supervise and operate Superficial Radiotherapy rather than a complicated coordination of care with a Radiation Oncologist and your Dermatologist. Due to the required involvement of physicists, radiation therapists, and a Radiation Oncologist, Xoft™ Electron Brachytherapy may be several times more costly than Superficial Radiotherapy provided by SRT-100™.
If you have any additional questions, please contact the office at (925) 328-0255 or email staff@CalDermCare.com
*Patient education matters to us. The information on this page has been reviewed by the board-certified dermatologists of California Dermatology Care. If you have any questions about our procedures or treatments, please get in touch with us today.
View Before & After Photos









